Coccydynia Treatment: Causes, Symptoms, and Effective Relief
Introduction
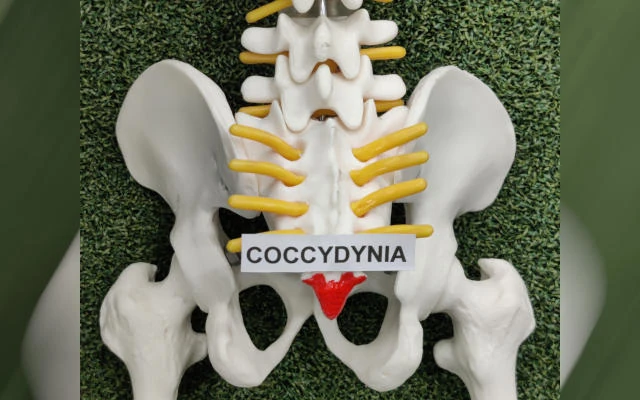
Coccydynia, also known as tailbone pain, is discomfort or soreness felt at the very bottom of your spine. This small triangular bone (the coccyx) supports your body when you sit, helps maintain posture, and connects to important muscles in your pelvic floor. When this area becomes injured, strained, or inflamed, even simple actions — like sitting, bending, or getting up from a chair — can cause pain.
The good news? Most people recover completely with the right coccydynia treatment, especially when it includes physiotherapy for tailbone pain and a few posture and lifestyle changes.
Common Causes of Coccydynia
- Trauma or Falls: A direct fall onto the buttocks is the most common cause. Even minor trauma can lead to bruising or dislocation.
- Childbirth: Difficult or instrument-assisted deliveries can strain or dislocate the coccyx.
- Poor Sitting Posture: Prolonged sitting on hard or uneven surfaces increases tailbone pressure.
- Obesity or Rapid Weight Loss: Both extremes can alter sitting biomechanics.
- Degenerative Changes: Age-related wear or inflammation in coccyx joints.
- Rare Causes: Tumors, infections, or abnormal coccyx shapes (like a sharp forward curve).
How Severe Is It?
Tailbone pain can range from mild to chronic:
| Type | Symptoms | What It Means |
|---|---|---|
| Mild | Pain after long sitting | Usually posture-related, improves with early care |
| Moderate | Pain while sitting, standing, or using stairs | Often due to inflammation or joint irritation |
| Severe / Chronic | Constant pain radiating to buttocks or legs | May involve coccyx dislocation or long-standing irritation |
Diagnosis — How It’s Confirmed
Your doctor or physiotherapist will begin with a detailed history and physical exam. They’ll check your posture, muscle tightness, and how your coccyx moves.
Clinical Evaluation
A doctor or physiotherapist will assess:
- Posture and movement: How you sit, stand, and transition positions.
- Palpation: Gentle pressure over the coccyx to check for tenderness, spasm, or misalignment.
- Rectal exam (in chronic cases): To assess coccyx mobility.
Imaging Tests
- Dynamic X-rays: Show how the coccyx moves when sitting or standing.
- MRI: Detects inflammation, swelling, or rare causes like infection or fracture.
- CT scan: Used for trauma or post-surgical evaluation.
A proper diagnosis helps your physiotherapist create a personalized Coccydynia treatment plan instead of a one-size-fits-all approach.
Treatment Options
Most patients recover fully through non-surgical Coccydynia treatment focused on reducing inflammation and correcting mechanical stress.
Conservative Management
- Cushions: Use a donut or wedge cushion to take pressure off the tailbone.
- Posture correction: Sit tall, avoid leaning backward, and take frequent breaks.
- Heat/Ice therapy: Helps relieve pain and muscle tension.
- Medication: Short-term NSAIDs or muscle relaxants for acute inflammation.
- Lifestyle changes: Maintain a healthy weight, avoid hard seating surfaces, and take sitting breaks every 30–45 minutes.
Medical Management
If pain persists:
- Injections: Corticosteroid or ganglion impar injections reduce inflammation.
- Shockwave therapy or PRP: Promote healing in chronic cases.
- Surgery (Coccygectomy): Rarely needed — only in severe cases unresponsive to other treatments.
Physiotherapy Management for Coccydynia
Physiotherapy plays a central role in both pain relief and long-term recovery. Evidence shows that physiotherapy for tailbone pain can reduce pain intensity by up to 80% and restore full sitting tolerance in 8–12 weeks.
Phase 1: Pain Relief and Inflammation Control
- Modalities: Ultrasound, IFT, or Shockwave Therapy for pain reduction.
- Cushion Support: Use U-shaped or wedge cushions to relieve coccyx pressure.
- Ergonomic Training: Learn proper sitting posture and workstation setup.
- Manual Therapy:
- Coccygeal and sacrococcygeal mobilization
- Soft-tissue and myofascial release for gluteal and pelvic floor muscles
- Intrarectal manipulation (performed by trained physiotherapists)
Phase 2: Mobility Restoration and Postural Correction
- Stretching exercises: Target piriformis, iliopsoas, and levator ani to relieve pelvic tension.
- Pelvic floor coordination: Gentle contraction and relaxation to reduce internal stress.
- Lumbar–pelvic alignment drills: Strengthen spinal stabilizers and retrain posture.
- Breathing exercises: Improve diaphragm–pelvic floor synergy for better spinal stability.
Phase 3: Strengthening and Functional Rehabilitation
- Core stabilization: Focus on transverse abdominis and multifidus activation.
- Gluteal and hip strengthening: Enhances pelvic support and sitting tolerance.
- Dynamic balance training: Re-educates pelvic coordination for everyday activities.
- Gradual sitting reintroduction: Structured sitting tolerance program using cushions.
Phase 4: Maintenance and Prevention
- Home exercise program: Continue daily mobility and strengthening routines.
- Regular breaks: Avoid sitting beyond 45 minutes continuously.
- Monitor ergonomic habits: Keep hips slightly higher than knees while sitting.
- Follow-ups: Periodic reviews to ensure long-term stability and prevent recurrence.
Prognosis and Long-Term Outcomes
With early physiotherapy for tailbone pain, most patients recover within 6–10 weeks. Chronic cases may take longer but still respond well to comprehensive Coccydynia treatment combining manual therapy, posture retraining, and strengthening.
Studies show that up to 90% of cases recover without surgery, especially when treated early and consistently.
Role of Physiotherapist
A physiotherapist doesn’t just treat the pain — they restore function and prevent recurrence.
Their role includes:
- Identifying root cause: Whether due to posture, trauma, or muscle imbalance.
- Applying manual techniques: Mobilization, release, and realignment of the coccyx.
- Educating on posture: Teaching ergonomic corrections to prevent flare-ups.
- Designing personalized plans: Based on lifestyle, occupation, or postpartum needs.
- Tracking progress: Using pain scales, movement assessments, and periodic evaluations.
Key Takeaway
Coccydynia treatment is most effective when started early. You don’t have to live with tailbone pain — with guided physiotherapy for tailbone pain, ergonomic adjustments, and lifestyle correction, long-term recovery is completely achievable without surgery.
References:
Physiopedia – www.physio-pedia.com
Archives of Physiotherapy (2025) – Effectiveness of physical therapy interventions for coccydynia
International Journal of Musculoskeletal Disorders (2018) – Anatomy, etiology, diagnosis, treatment
Journal of Manual and Manipulative Therapy (2013) – Conservative interventions for coccydynia
American Academy of Orthopaedic Surgeons – www.aaos.org
Mayo Clinic – www.mayoclinic.org
NHS – www.nhs.uk
FAQs on Coccydynia
How long does coccydynia last?
Most cases resolve in weeks to months. Chronic cases may last >6 months but can improve with therapy.
Can coccydynia be cancer?
Rarely, tumors like chordoma can cause coccyx pain. Imaging helps rule this out.
Is sitting on a soft cushion enough?
Special donut or wedge cushions reduce pressure, but exercise and posture correction are also important.
Can pregnancy cause coccydynia?
Yes. Childbirth is a common trigger due to stretching and trauma of the pelvic region.
Should I avoid exercise?
No. Light stretching, pelvic floor exercises, and core strengthening usually help recovery.