Sciatica: Causes, Symptoms, and Treatment Options
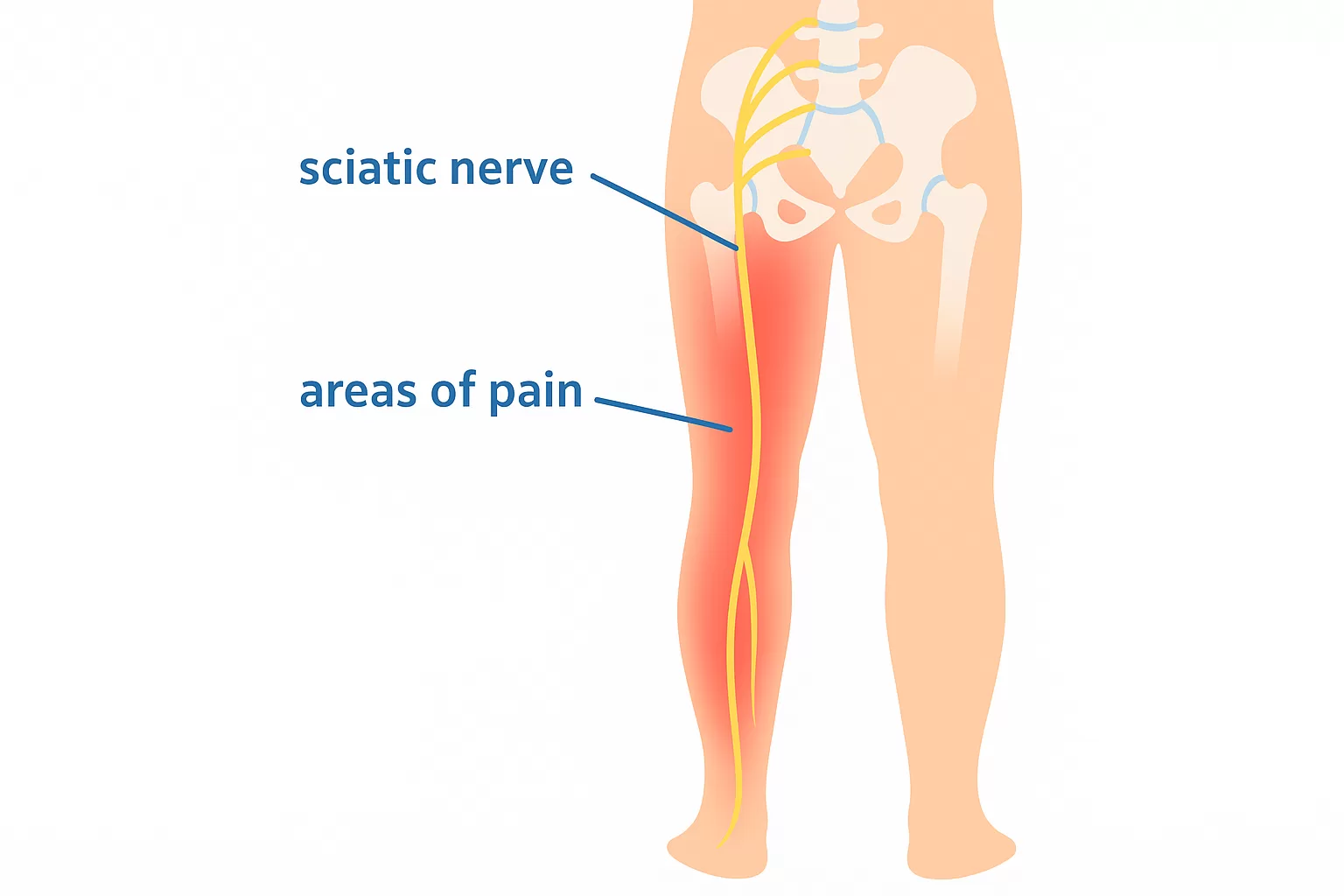
If you feel sharp pain running from your lower back into your leg, you may have sciatica. Unlike regular back pain, sciatica happens when a nerve in your lower spine gets irritated or pressed. This usually occurs at the L4, L5, or S1 level. That nerve connects to the sciatic nerve, the largest nerve in your body. It runs through the buttock, thigh, and foot.
The most common cause is a slipped or herniated disc. However, sciatica can also come from arthritis, spinal canal narrowing (stenosis), or tight buttock muscles called piriformis syndrome. As a result, pain may spread down the leg and sometimes reach the foot. For anyone struggling with these symptoms, starting a guided Sciatica Treatment plan early with a physiotherapist can help prevent chronic pain and long-term disability.
How Bad Is My Sciatica?
Sciatica doesn’t feel the same for everyone. For some, it’s mild and tolerable. For others, it can be very painful. That’s why physiotherapists often classify sciatica into four stages depending on severity and symptoms.
Level 1: Mild Sciatica (Early Nerve Irritation)
- Pain is mild but noticeable.
- It often feels like a dull ache with tingling.
- Most people can continue their daily routine with small changes.
Treatment: Keep moving, avoid long bed rest, try gentle stretches, and apply ice or heat. Over-the-counter pain relief may help. Gentle exercises under the expert guidance of physiotherapy for sciatica at this stage can control inflammation and prevent worsening.
Level 2: Moderate Sciatica (Ongoing Compression)
- Pain becomes sharper and often travels below the knee.
- Weakness or numbness may appear.
- Daily activities slowly become harder.
Treatment: At this stage, physiotherapy for sciatica includes core strengthening, posture training, and nerve mobility exercises to reduce strain on the nerve. In addition, healthy weight management and avoiding heavy lifting protect your back.
Level 3: Severe Sciatica (Weakness or Numbness)
- Pain is constant and intense.
- Muscle weakness or loss of reflexes may appear.
Treatment: Intensive sciatica treatment through structured physiotherapy can help relieve pain and restore function. If symptoms persist, injections may be advised, and further evaluation by a spine specialist might be needed.
Level 4: Advanced Sciatica (Emergency Stage)
- Pain becomes extreme and difficult to manage.
- Severe weakness or loss of bladder or bowel control may occur.
Treatment: This stage is a medical emergency, and surgery may be necessary to relieve pressure on the nerve.
Can Sciatica Be Managed Without Surgery?
Yes, in most cases. In fact, most people improve within three months using simple, conservative treatments. Non-surgical sciatica treatment and physiotherapy in Chennai and other structured rehabilitation programs have shown excellent recovery results for many patients. Surgery is typically reserved for severe or persistent cases.
The most effective options include:
- Physiotherapy for sciatica — targeted exercises like McKenzie extensions, nerve gliding, and core strengthening.
- Education — learning safe postures for sitting, standing, and lifting.
- Lifestyle changes — staying active, maintaining a healthy weight, and quitting smoking.
- Pain relief — short-term use of NSAIDs, along with heat or ice therapy.
- Hydration — drinking enough water to support spinal disc and nerve health.
How a Physiotherapist Can Help
During your visit, the physiotherapist will:
- Take your detailed history — when pain started, what worsens or relieves it.
- Test flexibility, strength, reflexes, and nerve tension using exams like the straight leg raise test.
- Suggest scans such as MRI if needed to confirm diagnosis.
Once assessed, a personalized sciatica treatment plan will be created to:
- Reduce pain and nerve irritation.
- Improve movement and restore confidence.
- Strengthen your core and spinal muscles.
- Teach you how to protect your back during daily activities.
Why Physiotherapy Is a Smart Choice
Physiotherapy for sciatica provides effective pain relief without the need for strong medications or invasive procedures. It enhances mobility, posture, and stability while lowering the risk of recurrence.
Moreover, physiotherapy is cost-effective compared to surgery and empowers patients with self-care strategies. By following a structured home program, most people experience lasting relief and improved function.
The Bottom Line
Sciatica can be painful and disruptive, but recovery is absolutely possible. With timely sciatica treatment, physiotherapy guidance, and lifestyle improvements, most people can return to a pain-free, active life.
By staying consistent with exercises and seeking help from an experienced physiotherapist, you can overcome sciatica safely and effectively — without surgery and making healthy lifestyle changes, you can recover from sciatica and return to a pain-free life and return to a pain-free life.
FAQs on Sciatica
How do I know if my leg pain is really sciatica?
It’s usually sharp pain that travels from the lower back down the leg, often with tingling or numbness.
Can sciatica go away on its own?
Yes, most cases improve within 6–12 weeks with simple care and activity.
Is walking good for sciatica?
Yes, gentle walking helps reduce stiffness and promotes healing.
When should I worry about sciatica?
If you have severe weakness, loss of bladder/bowel control, or worsening pain, seek urgent care.
Do I need an MRI right away?
No, unless symptoms are severe, persistent, or show red flags.
What exercises should I avoid?
Avoid heavy lifting, deep forward bends, and high-impact activities during flare-ups.
Will physiotherapy really help?
Yes, it eases pain, restores movement, and prevents recurrences.
Can lifestyle changes make a difference?
Absolutely—staying active, fit, and keeping good posture reduces future risk.